An Overview of Osteoporosis
Published: 02 March 2023

Published: 02 March 2023

Loss of bone density occurs naturally with age, but for the 900,000-plus Australians living with osteoporosis (Healthdirect 2020a), even a small fall or mechanical injury could mean a trip to hospital.
The aptly-named osteoporosis (meaning ‘bones with holes’) is a condition causing bones to become more porous due to loss of density (Better Health Channel 2019).
This decreased density means the bones are weaker, thinner and more fragile, which makes them more susceptible to breakage. As a result, the potential for injury - even from minor accidents - is increased (AIHW 2023).
When bones lose minerals (such as calcium) more quickly than they are able to be replenished, the density of those bones decreases (AIHW 2023). Peak bone density is reached between the age of 25 and 30, and after about 50 years of age, the body begins to break down more bone than it can rebuild (Better Health Channel 2019; MSK 2022).
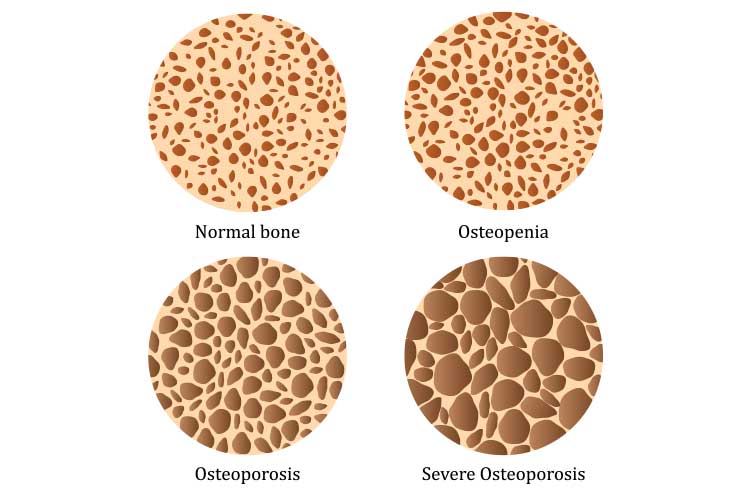
Loss of bone mineral density can be sorted into three categories depending on how far it has progressed.
These three categories are:
(MSK 2022)
Osteopaenia is a condition where there has been some loss of bone density, and bones are therefore weaker, but not frail enough to be considered osteoporosis (AIHW 2023).
In osteopaenia there is still some level of risk, but it is not as severe. Furthermore, an individual who has developed osteopaenia will not necessarily progress to having osteoporosis, but could be at greater risk of doing so (Healthdirect 2022).
According to the latest data from the Australian Bureau of Statistics (2018), 924,000 Australians (about 3.8% of the population) have self-reported having osteoporosis.
However, because it often doesn’t present with symptoms, osteoporosis is under-diagnosed and the exact prevalence is difficult to determine (AIHW 2023).
It’s generally more common among older populations, with prevalence increasing in females from about the age of 45 to 54, and in males from about the age of 55 to 64 (ABS 2018).
Osteoporosis is known as a ‘silent disease’ because there are usually no obvious symptoms until a fracture occurs (Better Health Channel 2019).
For this reason, it’s recommended that any person over 50 who suffers a broken bone from a minor accident or fall should be tested for osteoporosis (HBA 2020).
The following signs and symptoms may suggest osteoporosis:
(Mayo Clinic 2021)

There are certain risk factors that can be used to predict the occurrence of osteoporosis.
Naturally, the presence of osteopaenia could suggest progression to osteoporosis in the future.
Other risk factors include:
(Mayo Clinic 2021; HBA 2022; Healthdirect 2020a)
A bone density test known as the dual-energy x-ray absorptiometry (DXA) scan can be used to diagnose osteoporosis.
The scan uses radiation to measure bone tissue in the spine and hip and provides a ‘T-Score’, which categorises the individual’s bone density as either normal, osteopenia or osteoporosis. (MSK 2022).
Osteoporosis can lead to fractures in any bone, but the hip, spine and wrist are the most commonly fractured areas (MSK 2022).
In severe cases of osteoporosis, the bones are so thin that even coughing or bending over is enough to cause a fracture (Mayo Clinic 2021).
The fractures caused by osteoporosis can have a significant impact on the individual’s life, leading to chronic pain, disability, loss of independence or even death in some cases (AIHW 2023).
For this reason, osteoporosis has the potential to be severe or fatal if an accident occurs.
Once an individual has experienced an initial fracture due to osteoporosis, they have a 50% chance of experiencing another fracture (Arthritis NSW 2018).
This creates a ‘cascade effect’, which means the individual becomes more and more likely to suffer another fracture with each subsequent injury (Arthritis NSW 2018).
Osteoporosis can also cause the vertebrae to weaken and crumple, leading to spinal injuries without an accident having occurred (Mayo Clinic 2021).
Although the genetic risk factors of osteoporosis cannot be changed, it’s possible for an individual to reduce the possibility of developing osteoporosis by managing aspects of their lifestyle.
It’s important to ensure that the bones are thick and healthy from a young age before density begins to decrease.
The following are crucial to ensuring optimal bone health:
(MSK 2022; Healthdirect 2020a)

There is no cure for osteoporosis, but an individual may be prescribed medication to strengthen their bones and reduce the amount of density lost (Healthdirect 2020).
They may also be advised to make lifestyle changes. However, the most important way to manage osteoporosis is to focus on fall prevention and put measures into place to reduce the risk of having an accident (Healthdirect 2020b).
This includes reducing tripping hazards around the home, using walking sticks or frames to assist with steadiness and avoiding certain chores or tasks (Healthdirect 2020b).
After the onset of osteoporosis, it is important to stop the cascade effect from occurring.
Question 1 of 3
Once an individual has experienced their first fracture from osteoporosis, how likely is it that they will experience another one?