Complex Bowel Care: NDIS High Intensity Daily Personal Activities and Support Skills Descriptors
Published: 14 February 2023

Published: 14 February 2023

Workers employed by National Disability Insurance Scheme (NDIS) providers, who deliver supports to NDIS participants requiring complex bowel care, must be able to provide appropriate care.
This article has been updated in response to the release of Version 3 of the NDIS Practice Standards: High Intensity Support Skills Descriptors (HISSD), which came into effect on 1 February 2023.
Bowel care is a routine component of personal support that is imperative to a person’s quality of life (NDIS 2021a; NHS 2017).
However, NDIS participants at risk of severe constipation or faecal incontinence may require complex bowel care from support workers with a more specialised skill set (NDIS 2022).
Complex bowel care is a requirement of the NDIS Practice Standards under the High Intensity Daily Personal Activities Module.
This Practice Standard aims to ensure that NDIS participants requiring complex bowel care receive appropriate support that is relevant and proportionate to their individual needs (NDIS 2021).
Under these standards, care providers must meet the following quality indicators:
(NDIS 2021b)
Complex bowel care may be required for NDIS participants living with:
(NDIS 2022)
A participant who is receiving non-routine treatment such as non-routine pro re nata (PRN) medication for bowel care may also require complex support (NDIS 2022).
The NDIS high intensity support skills descriptors are additional guidance specifically for NDIS workers who are supporting participants with high intensity daily personal activities (HIDPA). Many of these HIDPAs are high-risk and/or intimate care areas that require a high level of care, competency and communication. The high intensity support skills descriptors set out the skills and knowledge required for NDIS workers to effectively and safely support participants with HIDPAs (NDIS 2022).
The high intensity support skills descriptors have been updated as of 1 February 2023 in order to:
(NDIS 2023)
Workers providing complex bowel care under the NDIS should be able to:
(NDIS 2022)
Additionally, workers supporting a participant with a stoma in-situ should also be able to:
(NDIS 2022)
Read: The NDIS Practice Standards Explained
The NDIS Practice Standards establish the benchmark of performance, quality and safety that NDIS providers should meet in their delivery of supports and services (NDIS 2021b).
The Standards work alongside the NDIS Code of Conduct to inform NDIS participants about the quality they should be expecting from the supports and services they receive (NDIS 2021b).
The NDIS Code of Conduct sets out expectations for the behaviour of both NDIS workers and participants in order to promote safe and ethical service delivery. For more information of the NDIS Code of Conduct, see https://www.ndiscommission.gov.au/about/ndis-code-conduct.
Good bowel management is essential for a person’s physical health, self-esteem and overall quality of life (SCHN 2014).
Bowel conditions, particularly faecal incontinence, are highly stigmatised and can have severe social and emotional consequences (Duyos & Ribas 2019). Therefore, good bowel care can help support participants to gain more confidence and lead the life they choose.
Remember that bowel health is a highly personal and embarrassing subject for some people, so participants should always be treated with empathy and dignity.
Participants may have a variety of communication needs and preferences, such as the use of communication aids or devices, or access to resources in another language (NDIS 2022). Remember to individualise communication to ensure each participant’s needs and preferences are met.
For more information on communication supports, see the following Ausmed resources:
It’s essential to be aware of and follow infection control principles, including PPE, handwashing and disinfecting (NDIS 2022).
For more information on infection control, see Ausmed’s Training Module on Infection Prevention and Control.
Always work within your scope of practice and your role’s responsibilities. Refer to your manager and/or local policies and procedures for more clarity on your specific role and responsibilities if you are unsure.
Also see Ausmed’s Training Module on Scope of Practice: Care Workers.
When food is consumed, it breaks down in the stomach and passes through the intestines. The walls of the intestines then absorb nutrients from the food. The waste that remains is then passed through the colon and rectum and is excreted (Khan 2022).
Bowel motions are affected by a variety of factors, such as:
(Better Health Channel 2014; Healthy Eating Clinic 2020)
Complex bowel conditions in the NDIS high intensity support skills descriptors include:
(NDIS 2022)
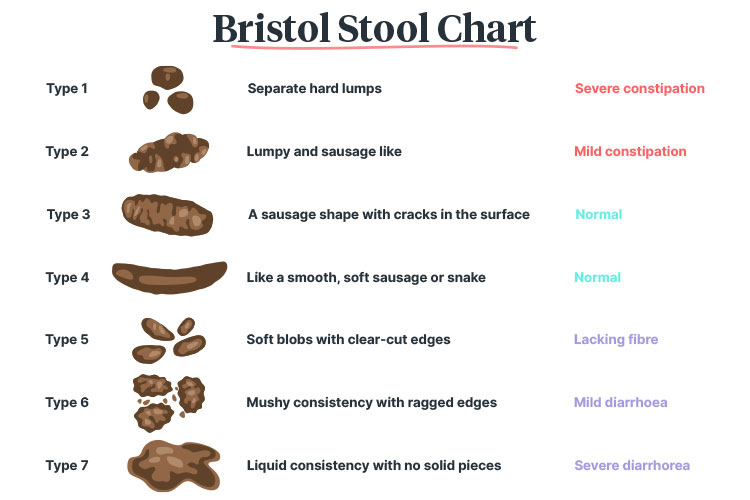
Constipation refers to difficulty defecating over an extended period of time. It is defined as the occurrence of less than three bowel movements per week (Premium Health 2022).
Someone who is constipated may simply have difficulty defecating (with a normal defecation frequency), or they may have a delayed colonic transit time of food from the mouth to the anus, which causes stools to become hard, dry and infrequent (Premium Health 2022; RCN 2019).
Common causes of constipation include:
(Better Health Channel 2014; Healthdirect 2022)
Signs and symptoms of constipation include:
(Better Health Channel 2014; Mayo Clinic 2021)
Someone experiencing faecal incontinence has difficulty with bowel control, causing involuntary loss of stools (RCN 2019).
Common causes of faecal incontinence include:
(Healthdirect 2020)
Signs and symptoms of faecal incontinence include:
(Healthdirect 2020)
Autonomic dysreflexia is a potentially life-threatening complication that can occur in people with spinal cord injury (typically a SCI above T6). It occurs in response to a strong sensory stimulus below the level of the injury, resulting in severe hypertension (ACI 2014).
Autonomic dysreflexia can be triggered by bowel issues such as constipation and faecal impaction. Therefore, good bowel care for participants with SCI is crucial in order to avoid this complication from occurring (ACI 2014).
Signs and symptoms of autonomic dysreflexia include:
(ACI 2014)
If you suspect autonomic dysreflexia in a participant you are caring for, you should immediately:
(ACI 2014)
Bowel issues can be managed in a variety of ways, including:
(NDIS 2022; Better Health Channel 2014)
A stoma is a surgically-created artificial opening, where a section or piece of the bowel is brought through the abdomen. This allows waste to be removed from the body directly through the end of the bowel into a collection bag (Healthdirect 2021; Cancer Council Victoria 2021).
There are two types of bowel stoma:
(Cancer Council Victoria 2021)
The waste that passes through the stoma is collected in a stoma bag, a pouch made from soft, waterproof material (Clinimed 2011).
This bag fits securely around the stoma and adheres to the abdomen using an attached or detachable flange, which is made from a breathable material and attaches to the skin using medical-grade adhesives. The type of bag needed will depend on the type of stoma (Clinimed 2011).
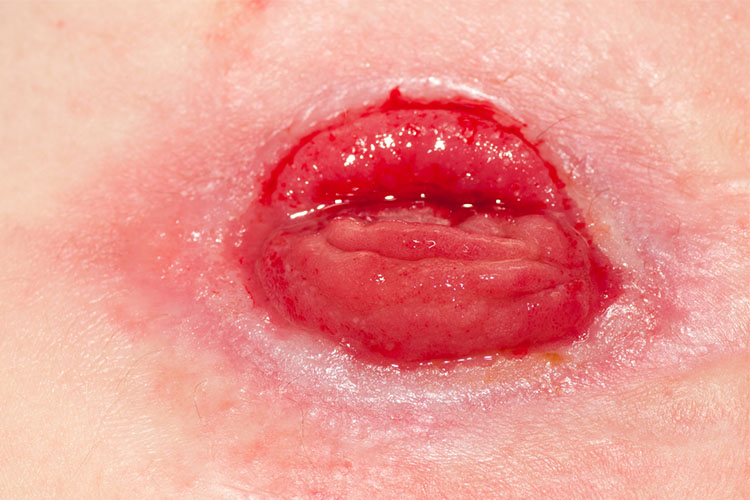
What should a heathy stoma look like?
(WACHS 2019)
How to care for skin around the stoma:
(WACHS 2019; Dansac 2018)
Issues at the stoma site:
The following signs and symptoms require escalation of care to an appropriately qualified medical practitioner:
(WACHS 2019; CHHS 2014; Finlay, Sexton & McDonald 2018; Better Health Channel 2011)
For more information on stomas and stoma care, see the Ausmed Course Acute Stoma Care.
You may have specific documentation and reporting responsibilities, such as handover, observations and incident reporting (NDIS 2022). Refer to your organisation’s policies and procedures for further information on what is required.
You should also be aware of the process for requesting a review of a participant’s care (NDIS 2022). Refer to your organisation’s policies and procedures for further information.
The participant should be referred to a health practitioner if they are experiencing the following complications:
(RCN 2019; NDIS 2021a)
Remember that bowel health may be embarrassing and highly personal for some people. Therefore, it is essential to communicate with participants empathetically.