Enteral Feeding Support: NDIS High Intensity Daily Personal Activities and Support Skills Descriptors
Published: 19 February 2023

Published: 19 February 2023

Note: This article is intended for NDIS workers and providers. For a more clinically-focused article on enteral feeding, see Caring for Enteral Tubes.
This article has been updated in response to the release of Version 3 of the NDIS Practice Standards: High Intensity Support Skills Descriptors (HISSD), which came into effect on 1 February 2023.
Workers employed by National Disability Insurance Scheme (NDIS) providers, who deliver supports to NDIS participants with an enteral (feeding) tube in place, must be able to provide appropriate support.
Enteral feeding is the delivery of liquid nutritional support through a tube inserted into the gastrointestinal tract. It is used for people who are unable to meet their nutritional requirements through oral intake. This may be because:
(DAA 2019)
Enteral feeding may complement oral intake or be used completely in place of oral intake (Dix 2018).
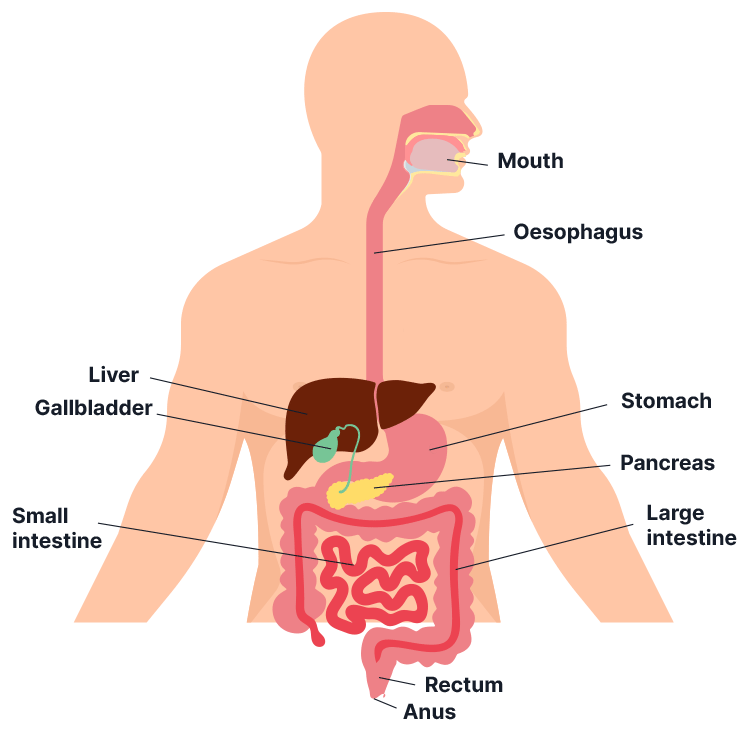
Enteral (Naso-Gastric Tube - Jejunum or Duodenum) Feeding and Management is set out in the NDIS Practice Standards under the High Intensity Daily Personal Activities Module.
This Practice Standard aims to ensure that NDIS participants who require enteral feeding and management receive nutrition, fluids and medicines that are appropriate, relevant and proportionate to their individual needs (NDIS 2021a).
Under these standards, NDIS providers must meet the following quality indicators:
(NDIS 2021)
In order to recieve enteral feeding support under the NDIS, a participant must have an enteral feeding and management support plan in place. This support plan should be developed in consultation with a health practitioner and may also involve other healthcare professionals such as dieticians, speech therapists or occupational therapists (NDIS 2022).
If the participant is to receive medications through an enteral feeding tube, they should also have a medication plan that outlines this (NDIS 2022).
The participant’s support plan may outline support needs such as:
(NDIS 2022)
The NDIS high intensity support skills descriptors are additional guidance specifically for NDIS workers who are supporting participants with high intensity daily personal activities (HIDPA). Many of these HIDPAs are high-risk and/or intimate care areas that require a high level of care, competency and communication. The high intensity support skills descriptors set out the skills and knowledge required for NDIS workers to effectively and safely support participants with HIDPAs (NDIS 2022).
The high intensity support skills descriptors have been updated as of 1 February 2023 in order to:
(NDIS 2023)
Workers providing enteral feeding support under the NDIS should be able to:
(NDIS 2022)
Workers supporting a participant with a gastrostomy should be able to:
(NDIS 2022)
Workers supporting a participant to administer medication through an enteral tube should be able to:
(NDIS 2022)
Read: The NDIS Practice Standards Explained
The NDIS Practice Standards establish the benchmark of performance, quality and safety that NDIS providers should meet in their delivery of supports and services (NDIS 2021b).
The Standards work alongside the NDIS Code of Conduct to inform NDIS participants about the quality they should be expecting from the supports and services they receive (NDIS 2021b).
The NDIS Code of Conduct sets out expectations for the behaviour of both NDIS workers and participants in order to promote safe and ethical service delivery. For more information of the NDIS Code of Conduct, see https://www.ndiscommission.gov.au/about/ndis-code-conduct.
Enteral support has a variety of benefits for people who would otherwise be unable to safely or adequately meet their nutritional requirements. These include reversing or preventing malnourishment, improving recovery from illness or surgery, and helping to optimise a person’s quality of life by ensuring they are nutritionally fulfilled, even without oral intake (WACHS 2019).
Therefore, appropriate and competent enteral feeding support is crucial for these participants.
Participants may have a variety of communication needs and preferences, such as the use of communication aids or devices, or access to resources in another language (NDIS 2022). Remember to individualise communication to ensure each participant’s needs and preferences are met.
For more information on communication supports, see the following Ausmed resources:
It’s essential to be aware of and follow infection control principles, including PPE, handwashing and disinfecting (NDIS 2022).
For more information on infection control, see Ausmed’s Training Module on Infection Prevention and Control.
Always work within your scope of practice and your role’s responsibilities. Refer to your manager and/or local policies and procedures for more clarity on your specific role and responsibilities if you are unsure.
Also see Ausmed’s Training Module on Scope of Practice: Care Workers.
There are three sites on the body where an enteral feeding tube can be inserted, and different route options for each site. The chosen site and route will depend on:
(DAA 2018)
The three sites on the body where an enteral feeding tube can be inserted are:
(WACHS 2019)
The different kinds of tubes that can be used to access each of these sites are:
(Ausmed 2021; Cancer Research UK 2020)
As a general rule, NG tubes are usually more appropriate for shorter durations of time, while PEG tubes can stay in situ for longer periods (Schwartz 2014).
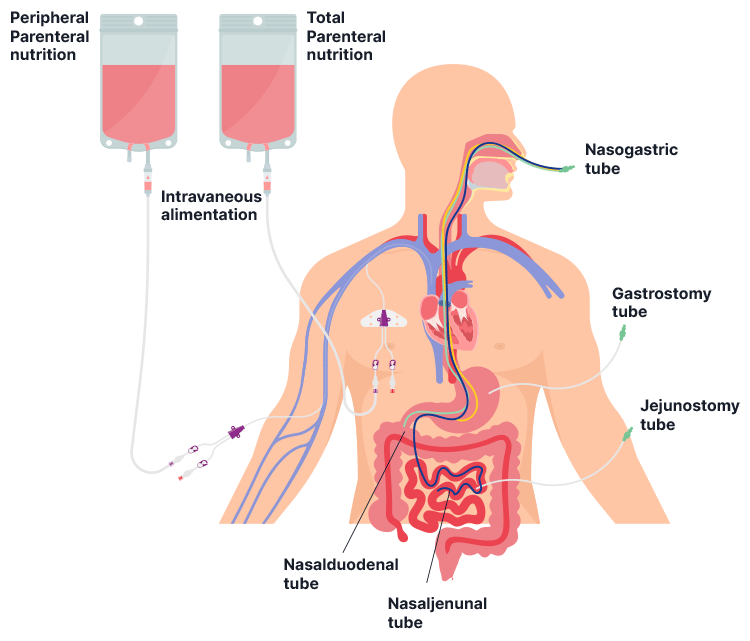
Feed can be administered using one of the following types of equipment:
(Queensland Health 2011)
Enteral feeding formulas contain a mixture of protein, fat, carbohydrate, fluid, vitamins and minerals, prescribed based on the the participant’s nutritional requirements (Queensland Health 2011).
Formulas can come in either a ready-to-use liquid form, or as a powder that needs to be mixed with fluid (Queensland Health 2011).
(Queensland Health 2011)
(WACHS 2019; Queensland Health 2011)
(Queensland Health 2011)
(Queensland Health 2011; WACHS 2019; NDIS 2022)
Participants should be positioned sitting up in a chair or lying down with their head raised to at least 30 degrees. They should never lie flat on their back (Queensland Health 2011).
After feeding, the participant should remain in an elevated position for 30 to 60 minutes (Queensland Health 2011).
Enteral feeding devices use alarms to alert to issues such as:
(Queensland Health 2011)
Alarms and methods for deactivating them will differ depending on the model of device being used. Always refer to the manufacturer’s directions.
If in your scope of practice, you may need to fix blocked or dislodged tubes. Refer to your organisation’s policies and procedures and your position description for more information.
In order to prevent blockage, tubes should be flushed:
(Queensland Health 2011)
The potential complications of enteral feeding include:
(WACHS 2019; Bapen 2016; CDHB 2022)
These complications can cause significant discomfort to participants and may develop into more serious concerns - for example, aspiration can lead to pneumonia (Mcilvoy 2019).
The following signs may be indicative of an issue:
(NDIS 2022)
People receiving enteral nutrition with little or no oral intake are at risk of issues such as dry mouth, oral infection and mouth discomfort. Therefore, maintaining good oral hygiene is essential in minimising the risk of these problems and optimising participants’ comfort (Bapen 2016).
You may have specific documentation and reporting responsibilities, such as handover, observations and incident reporting (NDIS 2022). Refer to your organisation’s policies and procedures for further information on what is required.
You should also be aware of the process for requesting a review of a participant’s care (NDIS 2022). Refer to your organisation’s policies and procedures for further information.
A participant should be referred to your manager or an appropriately qualified healthcare practitioner (refer to your organisation’s policies and procedures) if they are experiencing any of the following complications:
(NDIS 2022)
Workers supporting a participant to administer medication through an enteral tube are required to also have knowledge on:
(NDIS 2022)
Workers supporting a participant with a gastrostomy are required to also have knowledge on:
(NDIS 2022)
NDIS providers should ensure that staff supporting participants with enteral feeding have the skills and knowledge outlined by the Skills Descriptors, and are reviewed annually for competency (NDIS 2022).