Third and Fourth Degree Perineal Tears Explained
Published: 13 February 2024
Published: 13 February 2024

Perineal tears, while common and usually minor, may cause significant complications if the injury is extensive.
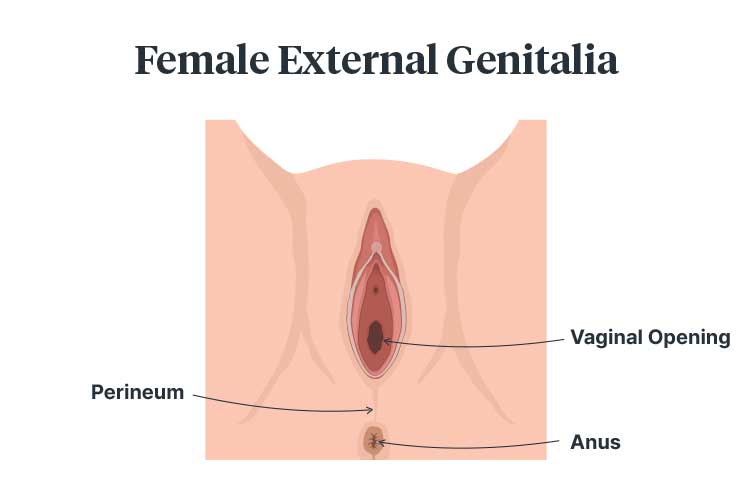
A perineal tear occurs when the perineum - the area between the vagina and anus - is injured during childbirth (ACSQHC 2021).
Tears are caused by the fetal head stretching the vagina and perineum during delivery (RCOG 2019a).
While perineal tears are common, occurring in over 85% of vaginal births (Goh et al. 2018), most do not result in serious injury (ACSQHC 2021).
However, third and fourth degree perineal tears (also known as severe perineal tears or obstetric anal sphincter injuries), which are experienced by approximately 3% of people giving birth vaginally and 5% of people giving birth vaginally for the first time, are more serious and may lead to complications (ACSQHC 2021).
Third and fourth degree perineal tears may adversely affect physical, psychological and sexual wellbeing, and sometimes require surgery (ACSQHC 2021).
While it is possible to reduce the risk of experiencing a perineal tear, they are not completely preventable. However, with effective treatment, including specialised care (if required), most patients who experience tears are able to recover (ACSQHC 2021).
There are three categories of risk factors for perineal tears: maternal, fetal, and intrapartum (Goh et al. 2018).
(ACSQHC 2021; Goh et al. 2018)
(ACSQHC 2021)
(ACSQHC 2021; Goh et al. 2018)
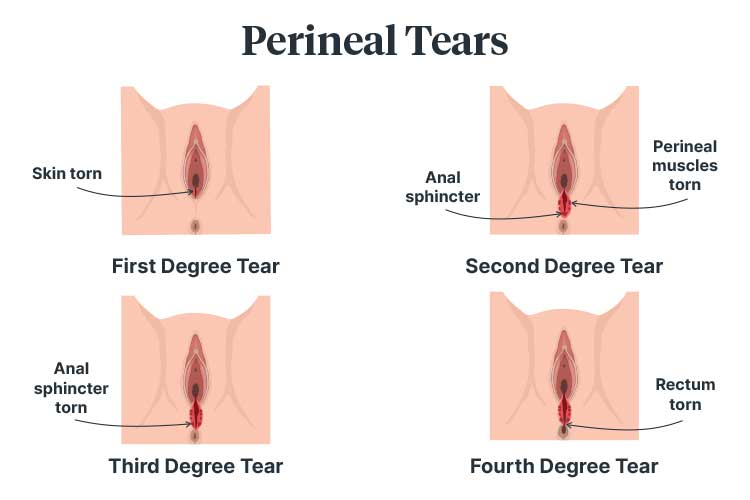
Perineal tears are classified depending on the extent of the injury, with first degree tears being the most minor and fourth degree tears being the most severe (Queensland Health 2021a).
| Degree | Description | Treatment | |
|---|---|---|---|
| 1 | A shallow injury that affects the skin only of the vaginal mucosa or perineum. | May heal on its own or require stitches. Recovery is usually within the first few weeks or months after birth. | |
| 2 | An injury that affects the perineal muscles. | Usually requires stitches. Recovery is usually within the first few weeks or months after birth. | |
| 3 | An injury that affects the perineal muscles and anal sphincter muscles. There are three sub-classifications: | Usually requires stitches given in an operating theatre under anesthetic. | |
| 3A | Less than 50% of the external anal sphincter is injured. | ||
| 3B | More than 50% of the external anal sphincter is injured. | ||
| 3C | Both the external and internal anal sphincters are injured. | ||
| 4 | An injury to the perineum that extends through the anal sphincter to the anal epithelium. | Usually requires stitches given in an operating theatre under anesthetic. |
(Goh et al. 2018; Queensland Health 2021a, b; RCOG 2019b)
Those who experience third and fourth degree perineal tears may experience short-term or long-term adverse effects including:
(ACSQHC 2021; Ramar & Grimes 2023)
An episiotomy involves making an incision in the perineum to increase the diameter of the vaginal opening. This creates more space for the fetal head, reducing the risk of a third or fourth degree perineal tear (ACSQHC 2021; Goh et al. 2018).
The incision made in an episiotomy is similar to a second degree perineal tear (Queensland Health 2021a).
An episiotomy should be performed using a medio-lateral technique with an incision angle of 60° from the midline (ACSQHC 2021).
An episiotomy is indicated in the following situations:
(ACSQHC 2021)
With the above situations as exceptions, the routine use of episiotomy is not recommended (SCV 2019).
Perineal tears are usually repaired using stitches, with third and fourth degree tears being repaired in an operating theatre under anaesthetic (as this facilitates anal sphincter relaxation) (Goh et al. 2018).
When a perineal tear is being repaired:
(Goh et al. 2018; ACSQHC 2021)

This may include:
(Goh et al. 2018; ACSQHC 2021)
Following repair, the patient may need to be referred to an obstetrician if they are experiencing:
(Goh et al. 2018)
Strategies to reduce the risk of experiencing a perineal tear include:
(Queensland Health 2021a; ACSQHC 2021)
During labour and birth, strategies include:
(Queensland Health 2021a; ACSQHC 2021)
The Third and Fourth Degree Perineal Tears Clinical Care Standard was released by the Australian Commission on Safety and Quality in Health Care in 2021.
This standard aims to decrease unwarranted clinical variation in cases of third and fourth degree perineal tears and ensure patients who have experienced third or fourth degree perineal tears receive appropriate care that enhances physical and psychological recovery.
The standard comprises the following seven Quality Statements:
| Quality Statement 1: Information, shared decision making and informed consent | Patients are appropriately informed about the possibility of experiencing a third or fourth degree perineal tear by the third trimester. This information is individualised and provided to the patient in a way they can understand. |
| Quality Statement 2: Reducing risk during pregnancy, labour and birth | During pregnancy, patients are advised on how to reduce the risk of a severe tear. During labour, the clinician uses evidence-based strategies to reduce the risk. |
| Quality Statement 3: Instrumental vaginal birth | When an instrumental delivery is indicated, the clinician considers clinical need and the potential benefits and risks (including the risk of a severe perineal tear). |
| Quality Statement 4: Identifying third and fourth degree perineal tears | Patients are examined after vaginal birth for perineal tears by an appropriately qualified clinician. Any identified tears are appropriately classified and documented. |
| Quality Statement 5: Repairing third and fourth degree perineal tears | Third and fourth degree tears are quickly repaired in an appropriate environment by an appropriately qualified clinician. |
| Quality Statement 6: Postoperative care | Patients receive postoperative care after repair of a severe tear. This should comprise debriefing, physiotherapy and psychosocial support. |
| Quality Statement 7: Follow-up care post-discharge | Patients receive individualised follow-up care after repair of a severe tear to optimise physical, emotional, psychological and sexual health. They are referred to a specialist if required. |
(ACSQHC 2021)