Umbilical Cord Clamping: How Long Should You Wait?
Published: 20 February 2023

Published: 20 February 2023

Until recently, clamping and cutting the umbilical cord immediately after birth (within 30 seconds) was considered to be standard practice to allow urgent medical care to be given (The University of Sydney 2021; De Bernando 2021).
Today, however, following extensive research, the practice of immediate clamping has largely been replaced by delayed cord clamping (DCC), which has been shown to have significant benefits for the infant and is now recommended in most circumstances (The University of Sydney 2021; Tommy’s 2021).
After birth, the placenta continues to pulsate and transfers blood, oxygen, and stem cells to the infant (Tommy’s 2021).
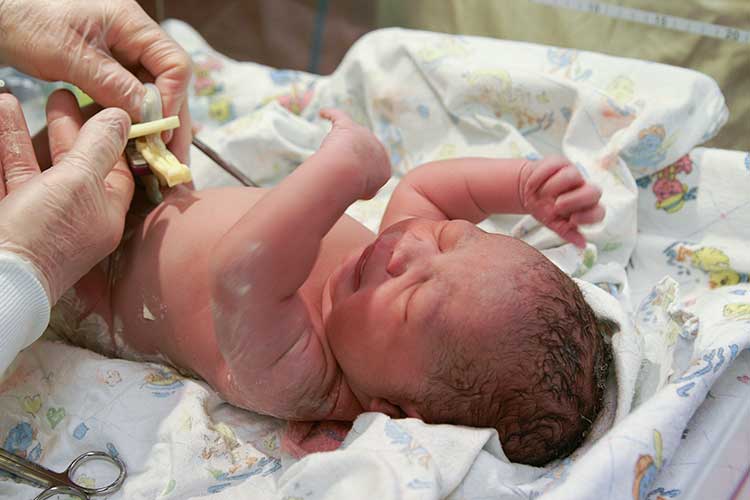
Cord clamping is the process of binding the umbilical cord using a nipper, which restricts this blood flow between the infant and the placenta. The umbilical cord is then cut (De Bernando 2021).
In delayed cord clamping (DCC), rather than clamping the cord immediately after birth, the midwife waits until the cord has stopped pulsating before clamping it (Tommy’s 2021).
The National Institute for Health and Care Excellence (2017) recommends that cord clamping occurs no earlier than one minute following birth, unless there are concerns about the cord’s integrity of the infant’s heartbeat.
This is supported by the latest Australian research, which indicates that healthcare professionals should aim to wait at least 60 seconds before clamping the cord (The University of Sydney 2021).
Note that the cord should ideally be clamped within five minutes (Tommy’s 2021).
Research has found a variety of benefits of DCC for infants. These include:
(The University of Sydney 2021; NICE 2017; Tommy’s 2021)
Other potential benefits include:
(Gruneberg & Crozier 2015)
Situations where DCC may not be appropriate include:
(Tommy’s 2021)

An alternative method that can provide newborns with the necessary additional blood volume is umbilical cord milking (UCM).
It’s a simple technique, performed by gently grasping the uncut umbilical cord and squeezing several times from the placenta towards the infant. In contrast to delayed cord clamping, milking provides a placental transfusion without postponing resuscitation and can be completed as quickly as immediate cord clamping (Tommy’s 2021).
Ibrahim et al. (2017) suggest that this can be an efficient method of improving blood volume, particularly in premature infants who may need resuscitation, as well as infants delivered by caesarean birth.
Despite immediate clamping of the umbilical cord being standard practice until recent years, delayed cord clamping is now routine and is recommended for most births due to the numerous benefits it provides.