Good mouth care is important - not only for oral health but also for general health and wellbeing.
Poor dental health has been linked to heart disease, stroke, diabetes and even certain cancers (Jordão et al. 2019).
While oral health issues are not inevitable with age, older adults over 50 are significantly more likely to experience problems with their teeth and gums (Ngai 2019).
We need to consider the mouth care we are delivering to our older patients - particularly those who are residents in aged-care facilities, where oral and dental disease are prevalent (Health.vic 2022).
Hospitalisation is also linked to a deterioration in oral health, especially for patients who are intubated (Terezakis et al. 2011).
Oral Health Under the Strengthened Aged Care Quality Standards
Standard 5: Clinical Care - Outcome 5.4: Comprehensive care under the strengthened Aged Care Quality Standards requires aged care providers to monitor changes to oral health and refer older people to relevant oral health services if needed (ACQSC 2024).
Additionally, Outcome 5.5: Clinical Safety (Action 5.5.7) requires providers to establish processes for optimising older people’s oral health and decreasing deterioration by:
- Facilitating access to oral health practitioners for assessment upon the commencement of care, routinely and when needed
- Recognising and addressing deteriorations in oral health
- Assisting older people with daily oral hygiene where required.
(ACQSC 2024)
What is Oral Health?
Oral health can be defined as ‘the ability to eat, speak and socialise without discomfort or active disease in the teeth, mouth or gums’ (AIHW 2023).
It is integral to a person’s overall wellbeing and quality of life and contributes significantly to positive ageing (SA Health 2019).
Oral health comprises:
- Lips
- Tongue
- Gums and tissues
- Saliva
- Natural teeth
- Dentures
- Oral cleanliness
- Dental pain.
(SA Health 2015)
Oral Health and Ageing

There are a number of reasons why older adults are more likely to experience oral health issues.
Older adults are becoming increasingly more likely to retain their natural teeth, which require routine care. Due to functional decline, cognitive impairment, frailty, comorbidities and other issues commonly associated with ageing, older adults may become less able to self-manage their oral health. This, in turn, increases the risk of disease or infection (SA Health 2015).
There are also physiological changes to the mouth that occur with age. Teeth become brittle and more prone to chipping or cracking, allowing bacteria to enter through the damaged areas and cause decay. The production of saliva - which helps to clear food particles, reduce bacteria and neutralise damaging acids - also decreases, leaving the mouth dry and the teeth more vulnerable to decay. Dry mouth, also known as xerostomia, affects about 25% of older adults (Ngai 2019).
Medicines may worsen the issue, as polypharmacy and common medicine classes can cause xerostomia as a side effect. This can lead to decay, oral infection or even aspiration pneumonia. (SA Dental 2022).
Other factors that contribute to oral decline include a weakened immune system, lifestyle risks such as smoking, drinking and diet, and menopause - which may cause xerostomia or tooth loss (due to bone thinning) (Ngai 2019; MedlinePlus 2022).
On top of this, there are significant issues surrounding oral health in Australian residential care due to insufficient staffing, lack of training and oral hygiene being an overall ‘low priority’. This may exacerbate any existing oral health issues (Bite Magazine 2019).
The Effects of Poor Oral Health
Poor oral health can significantly affect an older adult’s wellbeing and quality of life.
- Oral pain and chewing difficulties may limit food choices and affect nutrition, which, in turn, may lead to incontinence, mobility issues or compromised skin integrity.
- Bad breath may affect an older adult’s self-esteem and willingness to socialise.
- Oral infections may complicate comorbidities such as diabetes, chronic heart failure and respiratory conditions.
- Pain and discomfort may affect mood and behaviour or cause sleeping difficulties.
- The older adult may generally feel depressed.
(SA Dental 2023)
Poor oral health may also cause:
- Bleeding gums
- Tooth decay
- Tooth loss
- Difficulty swallowing
- Difficulty speaking
- Compromised immune system
- Chronic infection
- Aspiration pneumonia
- Cardiovascular disease.
(SA Health 2015; SA Dental 2023)
Common Oral Health Issues
| Condition | Type of issue | Signs to look for |
| Angular Cheilitis | Lips |
|
| Glossitis | Tongue |
|
| Candidiasis (thrush) | Tongue |
|
| Gingivitis | Gums and tissues |
|
| Periodontitis | Gums and tissues |
|
| Oral cancer | Gums and tissues |
|
| Ulcers and sore spots | Gums and tissues |
|
| Stomatitis | Gums and tissues |
|
| Xerostomia | Saliva |
|
| Tooth decay | Natural Teeth |
|
| Root decay | Natural Teeth |
|
| Dentures that need repair or attention | Dentures |
|
| Poorly fitted dentures | Dentures |
|
| Poor oral hygiene | Oral cleanliness |
|
(Adapted from SA Health 2015)
Oral Health Assessment
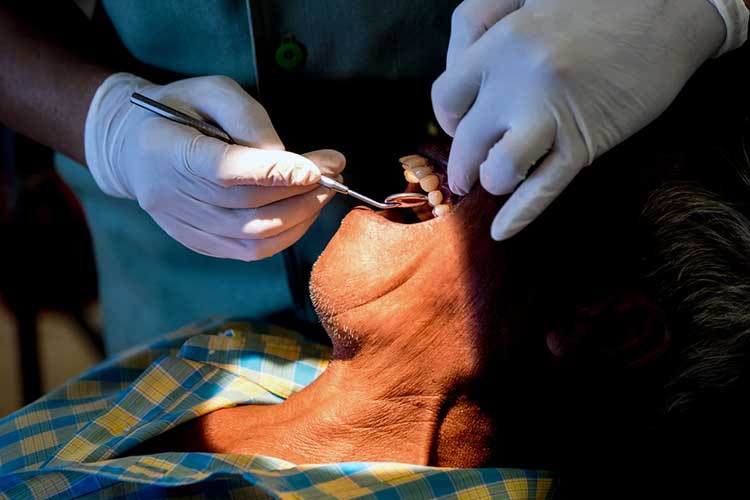
The best way for healthcare professionals to improve and care for the oral health of clients is via routine assessment.
Your facility should have a standardised assessment that all staff are trained on and are familiar with. It should assess and record all of the components of oral health:
- Lips - Assess for colour, chapping, swelling and lumps.
- Tongue - Assess for colour, coating, patches, swelling and ulcerated areas.
- Gum and tissues - Assess for colour, bleeding, loose teeth, gaps, swelling and patches.
- Saliva - How moist is the mouth? Does the patient complain of or notice dry mouth?
- Natural teeth - Look for cracks, decay, loose fillings, wear, biting mismatch.
- Dentures - Are they intact or worn down? Are there rough areas that could create ulcers?
- Cleanliness - Are the teeth clean? Is there any tartar, staining or food debris? Bad breath?
- Dental pain - Are there any behavioural, verbal or physical signs of pain? (e.g. chewing on one side of the mouth or wincing when biting).
This assessment should be carried out and recorded upon admission (or as close as possible to admission) and followed up on a frequent basis to ensure changes are monitored and can be treated in a timely manner.
Oral hygiene should be assessed twice per day (Health.vic 2022).
Developing a personalised oral health care plan for each resident is a key step in ensuring that good mouth care is maintained.
Once problem areas have been identified, it’s important to put a specific oral health care plan in place, ensuring necessary treatment is carried out and the overall health of the mouth can be improved.
Barriers to Oral Health
Some older adults may resist oral care, especially if they have dementia or delirium. They may:
- Be scared of being touched
- Refuse to open their mouth
- Not understand or respond to instructions
- Bite the toothbrush
- Grab or hit.
(SA Health 2015)
The following are some strategies for working with this behaviour and helping the client feel comfortable while performing oral assessment and care:
- Speak clearly to the client, using words they understand. Be reassuring. Recognise any signs that the client is having difficulty understanding you (lack of response, disinterest, frustration etc.)
- Always explain what you are doing
- Interact with the client in a calm, friendly and patient manner
- Choose an appropriate environment that is comfortable for the client
- Maintain a routine
- Be aware of body language, eye contact and personal space
- If the client is afraid of being touched, you can try gently stroking their face. This may need to be repeated a number of times before performing oral care so that the client can build up their trust.
(SA Health 2015)
There are also techniques that can be attempted to improve access to the client’s mouth. Start by bridging and move down the list in order until you find a technique that works.
- Bridging: Show the toothbrush to the client and mime brushing your teeth. The aim is for the client to mirror your actions and brush their own teeth.
- Chaining: Gently bringing the client’s hand and toothbrush to their face and explain the action of brushing, encouraging them to take over.
- Hand-over-hand: Place your hand over the client’s hand and brush their teeth together.
- Distraction: Give the client a towel, cushion, activity board etc. as a distraction while you brush their teeth.
- Rescuing: If the attempts to perform oral care are not working and the relationship with the client is deteriorating, leave them be and ask someone else to take over later.
(SA Health 2015)

Develop an Oral Health Care Plan
An effective oral health care plan will involve the documentation of assessment findings along with any barriers to effective hygiene.
The plan should also include which tools and products are to be used to maintain good oral health care. These might include:
- Type of toothbrush and frequency
- Inter-dental care (flossing, interdental brushes etc.)
- Aids (mouth props, disclosing tablets etc.)
- Products (mouthwash, gum, mints, rinses etc.)
- Type of toothpaste to be used (high fluoride, sensitive, etc.)
- Dry mouth products or medicines.
It is important to involve the patient and encourage participation in their own oral health care as much as possible. It is crucial, therefore, that the following is also considered:
- Level of participation and whether any prompting might be required.
- The best caregiver to work with that patient, along with the best time and place for oral health care to be administered.
- Any choices available to the patient (e.g. flavour of toothpaste), rewards that will work, the desensitisation process to follow (if required) and anything else of relevance.
- Professional dental care that has been carried out, advised and planned for.
It is important that clients have access to professional dental care on a regular basis -f including routine examinations.
The final priority for any hospital or aged care facility is to ensure that training is appropriate for the oral needs of the clients.
Care of Dentures
Management of Dentures
Keep the following considerations in mind when caring for clients with dentures:
- Dentures should be brushed twice per day (morning and night).
- A denture brush should be used to clean dentures, as this provides better friction.
- Clean dentures should be kept in a container of fresh, cold water overnight so that the client can rest their gums.
- Dentures should be disinfected using a denture-soaking tablet.
(SA Health 2015)
How to Clean Dentures
In some cases, you may need to assist clients to clean their dentures.
When cleaning dentures, keep the following considerations in mind:
- Always perform hand hygiene before and after providing oral care. Don gloves before providing oral care.
- Dentures should be cleaned over a sink. In order to prevent the denture from breaking if dropped, put a bowl filled with water or washcloth in the base of the sink as protection.
- Dentures should be cleaned using a denture brush and either mild liquid soap or denture paste. Do not use regular toothpaste, as this can damage the surface of the denture and lead to irritation or fungal infection.
- Support the denture while cleaning it so that you don’t drop it.
- Holding a lower denture from end-to-end may apply too much force and cause breakage; hold it in the middle instead.
(SA Health 2015)
Cleaning a Lower Denture:
- Cradle the denture between your thumb and the base of your index finger.
- Brush all surfaces, removing dental plaque and any denture adhesive.
- If the denture has been re-lined with a soft cushion liner, clean it gently using a soft toothbrush.
(SA Health 2015)
Cleaning an Upper Denture:
- Support the denture between your thumb and fingers.
- Brush all surfaces, removing dental plaque and any denture adhesive.
- If the denture has been re-lined with a soft cushion liner, clean it gently using a soft toothbrush.
(SA Health 2015)
Cleaning a Partial Denture:
- Clean the metal clasps with a soft toothbrush
- Brush around the metal clasps gently. Ensure that you don’t bend or move them out of shape.
(SA Health 2015)
Practical Tips for Oral Health
Clients should be encouraged to:
- Clean their teeth or dentures twice per day (morning and night)
- Use a high fluoride toothpaste
- Use a soft toothbrush
- Stay hydrated
- Sip water if their mouth is dry
- Maintain a healthy diet
- Reduce sugar intake
- Visit a dentist regularly.
(SA Health 2015)
Conclusion
Oral health can have a dramatic effect on the overall health and wellbeing of clients.
Staff should be aware of oral health care, including barriers, obstacles, the effects of diet and medicines and how to perform the right care for the needs of each client.
Good oral health care should become ‘part and parcel’ of life at your ward or care facility rather than something you ‘have to do’, and is a case where leading by example can go a long way.
Test Your Knowledge
Question 1 of 3
Sophie is a resident at an aged-care facility. She has dementia and is afraid of being touched. Peter, a nurse, is trying to perform oral care. However, Sophie is not responding well to any of the techniques and is becoming distressed. What should Peter do?
Topics
Further your knowledge
References
- Aged Care Quality and Safety Commission 2024, Standard 5: Clinical Care, Australian Government, viewed 24 May 2024, https://www.health.gov.au/resources/publications/strengthened-aged-care-quality-standards-august-2025?language=en
- Australian Institute of Health and Welfare 2023, Older Australians, Australian Government, viewed 10 August 2023, https://www.aihw.gov.au/reports/older-people/older-australians/contents/health/health-selected-conditions#Oral%20health%20and%20disease
- Bite Magazine 2019, ‘An Age-old Problem: The Oral Health of the Elderly’, Bite Magazine, 10 August, viewed 10 August 2023, https://bitemagazine.com.au/an-age-old-problem-the-oral-health-of-the-elderly/
- Health.vic 2022, Oral and Dental Hygiene: Standardised Care Process, Victoria State Government, viewed 10 August 2023, https://www.health.vic.gov.au/sites/default/files/2022-12/standardise-care-oral-dental-hygiene.PDF
- Jordão, HWT, McKenna, G, McMenamin, ÚC, Kunzmann, A, Murray, LJ & Coleman, HG 2019, ‘The Association Between Self-reported Poor Oral Health and Gastrointestinal Cancer Risk in the UK Biobank: A Large Prospective Cohort Study’, United European Gastroenterology Journal, vol. 7 no. 9, viewed 10 August 2023, https://journals.sagepub.com/doi/10.1177/2050640619858043
- MedlinePlus 2022, Aging Changes in Teeth and Gums, U.S. Department of Health and Human Services, viewed 10 August 2023, https://medlineplus.gov/ency/patientinstructions/000951.htm
- Ngai, J 2019, ‘Oral Health for Older People’, Bupa Health Link, 14 May, viewed 10 August 2023, https://www.bupa.com.au/healthlink/conditions-and-treatments/common-illness-and-conditions/clinical-health-information/oral-health-for-older-people
- SA Dental 2023, Oral Health Care Planning, Government of South Australia, viewed 10 August 2023, https://www.dental.sa.gov.au/professionals/oral-health-resources/care-for-older-people-toolkit/acute-settings/oral-health-care-planning
- SA Dental 2022, Why Oral Health Care is Important, Government of South Australia, viewed 10 August 2023, https://www.dental.sa.gov.au/professionals/oral-health-resources/care-for-older-people-toolkit/why-oral-health-care-is-important
- SA Health 2015, Better Oral Health in Residential Care, Government of South Australia, viewed 10 August 2023, https://www.sahealth.sa.gov.au/wps/wcm/connect/09fa99004358886a979df72835153af6/BOHRC_Staff_Portfolio_Full_Version%5B1%5D.pdf?MOD=AJPERES&CACHEID=ROOTWORKSPACE-09fa99004358886a979df72835153af6-n5hOC7k
- SA Health 2019, South Australia’s Oral Health Plan 2019 - 2026, Government of South Australia, viewed 10 August 2023, https://www.sahealth.sa.gov.au/wps/wcm/connect/6513697c-c216-417e-be20-3ee3fa1ebcd5/2019-2026+SAOHP+FINAL+VERSION.pdf?MOD=AJPERES&CACHEID=ROOTWORKSPACE-6513697c-c216-417e-be20-3ee3fa1ebcd5-nKQfZUl
- Terezakis, E, Needleman, I, Kumar, N, Moles, D & Agudo, E 2011, The Impact of Hospitalization on Oral Health: A Systematic Review’, J Clin Periodontol., vol. 38, no. 7, viewed 10 August 2023, https://pubmed.ncbi.nlm.nih.gov/21470276/
 New
New 

